Abstract
Objective
To investigate whether the level of initial flow rate alters the work of breathing in chronic obstructive pulmonary disease (COPD) patients ventilated in pressure support ventilation (PSV).
Design
Prospective study.
Settings
Medical ICU in University hospital.
Patients
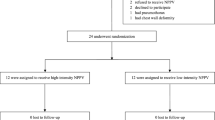
Eleven intubated COPD patients.
Methods
We modulated the initial flow rate in order to achieve seven different sequences. In each sequence, the plateau pressure was reached within a predetermined time: 0.1, 0.25, 0.50, 0.75, 1, 1.25 or 1.50 s. The more rapidly the pressure plateau was achieved, the higher was the initial flow rate. In each patient, the pressure support level was an invariable parameter. The order of the seven sequences for each patient was determined randomly.
Measurements and results
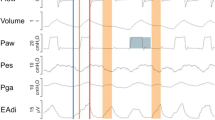
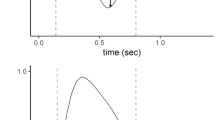
Ten minutes after application of each initial flow rate, we measured the following parameters: inspiratory work of breathing, electromyogram (EMG) of the diaphragm (EMGdi), breathing pattern, and intrinsic positive end-expiratory pressure (PEEPi). Comparison between the means for each sequence and each variable measured was performed by two-way analysis of variance with internal comparisons between sequences by Duncan's test. The reduction of the initial flow rate induced a progressive increase in the values of the work of breathing, EMGdi, and mouth occlusion pressure (P 0.1). In contrast, the reduction of the initial flow rate did not induce any significant change in tidal volume, respiratory frequency or PEEPi.
Conclusion
As the objective of PSV is to reduce the work of breathing, it seems logical to use the highest initial flow rate to induce the lowest possible work of breathing in COPD ventilated patients.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Brochard L, Rauss A, Benito S, Conti G, Mancebo J, Rekik N, Gasparetto A, Lemaire F (1994) Comparison of three methods of gradual withdrawal from ventilatory support during weaning from mechanical ventilation. Am J Respir Crit Care Med 150: 896–903
Tokioka H, Saito S, Kosaka F (1989) Comparison of pressure support ventilation and assist-control ventilation in patients with acute respiratory failure. Intensive Care Med 15: 364–367
Brochard L, Pluskwa F, Lemaire F (1987) Improved efficacy of spontaneous breathing with inspiratory pressure support. Am Rev Respir Dis 136: 411–415
Brochard L, Harf A, Lorino H, Lemaire F (1989) Inspiratory pressure support prevents diaphragmatic fatigue during weaning from mechanical ventilation. Am Rev Respir Dis 139: 513–521
Annat GJ, Viale JP, Dereymez CP, Bouffard YM, Delafosse BX, Motin JP (1990) Oxygen cost of breathing and diaphragmatic pressure-time index. Measurement in patients with COPD during weaning with pressure support ventilation. Chest 98: 411–414
Kacmarek RM (1988) The role of pressure support ventilation in reducing work of breathing. Respir Care 33: 99–120
Branson RD, Campbell RS, Davis K Jr, Johannigman JA, Johnson DJ, Hurst JM (1990) Altering flow rate during maximum pressure support ventilation: effects on cardiopulmonary function. Respir Care 35: 1056–1064
MacIntyre NR, Li-Ing Ho (1991) Effects of initial flow rate and breath termination criteria on pressure support ventilation. Chest 99: 134–138
Whitelaw WA, Derenne JP, Milic-Emili J (1975) Occlusion pressure as a measure of respiratory center output in conscious man. Respir Physiol 23: 181–199
Milic-Emili J, Mead J, Turner JM, Glauser EM (1964) Improved technique for estimating pleural pressure from esophageal balloons. J Appl Physiol 19: 207–211
Baydur A, Behrakis PK, Zin WA, Jaeger M Milic-Emili J (1982) A simple method for assessing the validity of the esophageal balloon technique. Am Rev Respir Dis 126: 788–791
Campbell EJM (1958) The pressure-volume diagram. In: Campbell EJM (ed) The respiratory muscles and the mechanics of breathing. Lloyd-Luke, London, pp 88–95
Guérin C, Coussa ML, Eissa NT, Corbeil C, Chassé M, Braidy J, Matar N, Milic-Emili J (1993) Lung and chest wall mechanics in mechanically ventilated COPD patients. J Appl Physiol 74: 1570–1580
European Community for Coal and Steel (1983) Standardization of lung function. Summary of recommendations. Bull Europ Physiopathol Respir 19 (Suppl 5): 7–10
Lopata M, Evanich MJ, Lourenco RV (1977) Quantification of diaphragmatic EMG response to CO2 rebreathing in humans. J Appl Physiol 43: 262–270
Lansing R, Savelle J (1989) Chest surface recording of diaphragm potentials in man. Electroencephalogr Clin Neurophysiol 72: 59–68
Goldman MD, Grimby G, Mead J (1976) Mechanical work of breathing derived from rib cage abd abdominal V-P partitioning. J Appl Physiol 41: 752–763
Tobin MJ, Guenther SM, Perez W, Lodato FR, Mador MJ, Allen SJ, Dantzker DR (1987) Konno-Mead analysis of ribcage-abdominal motion during successful and unsuccessful trials of weaning from mechanical ventilation. Am Rev Respir Dis 135: 1320–1328
Jaeger MJ, Otis AB (1964) Effects of compressibility of alveolar gas on dynamics and work of breathing. J Appl Physiol 19: 83–91
Fleury B, Murciano D, Talamo C, Aubier M, Pariente R, Milic-Emili J (1985) Work of breathing in patients with chronic obstructive pulmonary disease in acute respiratory failure. Am Rev Respir Dis 135: 822–827
Kimball WR, Leith DE, Robins AG (1982) Dynamic hyperinflation and ventilator dependence in chronic obstructive pulmonary disease. Am Rev Respir Dis 126: 991–995
Petrof BJ, Legaré M, Goldberg P, Milic-Emili J, Gottfried SB (1990) Continuous positive airway pressure reduces work of breathing and dyspnea during weaning from mechanical ventilation in severe chronic obstructive pulmonary disease. Am Rev Respir Dis 141: 281–289
Coussa ML, Guérin C, Eissa NT, Corbeil C, Chassé M, Braidy J, Matar N, Milic-Emili J (1993) Partitioning of work of breathing in mechanically ventilated COPD patients. J Appl Physiol 75: 1711–1719
Wheatley JR, West S, Cala SJ, Engel LA (1990) The effect of hyperinflation on respiratory muscle work in acute induced asthma. Eur Respir J 3: 625–632
Tantucci C, Corbeil C, Chassé M, Braidy J, Matar N, Milic-Emili J (1991) Flow resistance in patients with chronic obstructive pulmonary disease in acute respiratory failure. Effects of flow and volume. Am Rev Respir Dis 144: 384–389
Ward ME, Corbeil C, Gibbons W, Newman S, Macklem PT (1988) Optimization of respiratory muscle relaxation during mechanical ventilation. Anesthesiology 69: 29–35
Marini JJ, Rodriguez RM, Lamb V (1986) The inspiratory workload of patient-initiated mechanical ventilation. Am Rev Respir Dis 134: 902–909
Marini JJ (1986) Mechanical ventilation: taking the work out of breathing? Respir Care 31: 695–702
Kryger MH, Yacoub O, Anthonisen NR (1975) Effect of inspiratory resistance on occlusion pressure in hypoxia and hypercapnia. Respir Physiol 24: 241–248
Bellemare F, Grassino A (1982) Effect of pressure and timing of contraction on human diaphragm fatigue. J Appl Physiol 53: 1190–1195
Bellemare F, Grassino A (1982) Evaluation of human diaphragm fatigue. J Appl Physiol 53: 1196–1206
Proctor HJ, Woolson R (1973) Prediction of respiratory muscle fatigue by measurements of the work of breathing. Surg Gynecol Obstet 136: 367–370
Henning RJ, Shubin H, Weil MH (1977) The measurement of the work of breathing for the clinical assessment of ventilator dependence. Crit Care Med 5: 264–268
Fiastro JF, Habib MP, Shon BY, Campbell SC (1988) Comparison of standard weaning parameters and the mechanical work of breathing in mechanically ventilated patients. Chest 94: 232–238
Shapiro M, Wilson RK, Casar G, Bloom K, Teague RB (1986) Work of breathing through different sized endotracheal tubes. Crit Care Med 14: 1028–1031
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bonmarchand, G., Chevron, V., Jusserand, D. et al. Increased initial flow rate reduces inspiratory work of breathing during pressure support ventilation in patients with exacerbation of chronic obstructive pulmonary disease. Intensive Care Med 22, 1147–1154 (1996). https://doi.org/10.1007/BF01709328
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01709328