Abstract
Objective
The triggering capability of both the pressure and flow triggering systems of the Servo 300 ventilator (Siemens-Elema, Sweden) was compared at various levels of positive end-expiratory pressure (PEEP), airway resistance (Raw), inspiratory effort and air leak, using a mechanical lung model.
Design
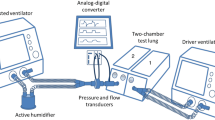
The ventilator was connected to a two bellows-in-series-type lung model with various mechanical properties. Lung complicance and chest wall compliance were 0.03 and 0.12 l/cmH2O, respectively. Raw was 5, 20 and 50 cmH2O/l/s. Respiratory rate was 15 breaths/min. To compare the triggering capability of both systems, the sensitivity of pressure and flow triggered pressure support ventilation (PSV) was adjusted to be equal by observing the triggering time at 0 cmH2O PEEP and 16 cmH2O of pressure support (PS) with no air leak. No auto-PEEP was developed. In the measurement of trigger delay, the PS level ranged from 16 to 22 cmH2O to attain a set tidal volume (VT) of 470 ml at a Raw of 5, 20 and 50 cmH2O/l/s. The PEEP level was then changed from 0, 5 and 10 cmH2O at a PS level of 17 cmH2O and Raw of 5 and 20 cmH2O/l/s, and the trigger delay was determined. The effect of various levels of air leak and inspiratory effort on triggering capability was also evaluated. Inspiratory effort during triggering delay was estimated by measurements of pressure differentials of airway pressure (Paw) and driving pressure in the diaphragm bellows (Pdriv) in both systems.
Measurements and results
There were no significant differences in trigger delay between the two triggering systems at the various PEEP and Raw levels. At the matched sensitivity level, air leak decreased trigger delay in both systems, and additional PEEP caused auto-cycling. A low inspiratory drive increased trigger delay in the pressure sensing system, while trigger delay was not affected in the flow sensing system. The Paw and Pdriv differentials were lower in flow triggering than in pressure triggering.
Conclusions
With respect to triggering delay, the triggering capabilities of the pressure and flow sensing systems were comparable with and without PEEP and/or high air-way resistance at the same sensitivity level, unless low inspiratory drive and air leak were present. In terms of pressure differentials, the flow triggering system may require less inspiratory effort to trigger the ventilator than that of the pressure triggering system with a comparable triggering time. However, this difference may be extremely small.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Branson RD (1994) Flow-triggering systems. Respir Care 39:138–144
Campbell RS, Branson RD (1993) Ventilatory support for the 90s: pressure support ventilation. Respir Care 38:526–537
Bernstein G, Cleary JP, Heldt GP, Rosas JF, Schellenberg LD, Mannino FL (1993) Response time and reliability of three neonatal patient-triggered ventilators. Am Rev Respir Dis 148:358–364
MacIntyre NR (1990) Importance of trigger sensitivity to ventilator response delay in advanced chronic obstructive pulmonary disease with respiratory failure. Crit Care Med 18:581–582
Sassoon CS (1992) Mechanical ventilator design and function: the trigger variable. Respir Care 37:1056–1068
Sassoon CS, Giron A, Ely E, Light R (1989) Inspiratory work of breathing on flow-by and demand-flow continuous positive airway pressure. Crit Care Med 17:1108–1114
Branson RD, Davis KJ, Jonson DJ, Campbell RS (1993) A comparison of flow and pressure triggering systems during CPAP (abstract). Respir Care 38:1244
Hirsh C, Kacmarek RM, Stanek K (1991) Work of breathing during CPAP and PSV imposed by the new generation mechanical ventilators: a lung model study. Respir Care 36:815–828
Kacmarek RM, Hess DR (1993) Airway pressure, flow and volume waveforms, and lung mechanics during mechanical ventilation. In: Kacmarek RM, Hess DR, Stoller JK (eds) Monitoring in respiratory care. Year Book Medical, St. Louis, pp 497–543
Takahashi T, Takezawa J, Kimura T, Nishiwaki K, Shimada Y (1991) Comparison of inspiratory work of breathing in T-piece breathing, PSV and pleural pressure support ventilation (PPSV). Chest 100:1030–1034
Capps JS, Ritz R, Pierson DJ (1987) An evaluation, in four ventilators, of characteristics that affect work of breathing. Respir Care 32:1017–1023
Marini JJ, Culver BH, Kirk W (1985) Flow resistance of exhalation valves and positive end-expiratory pressure devices used in mechanical ventilation. Am Rev Respir Dis 131:850–854
Chatburn R (1991) A new system for understanding mechanical ventilation. Respir Care 36:1123–1155
Christopher KL, Neff TA, Bowman JL, Eberle DJ, Irvin CG, Good JT (1985) Demand and continuous flow intermitent mandatory ventilation systems. Chest 87:625–630
Sanborn WG (1993) Microprocessorbased mechanical ventilation. Respir Care 38:72–108
Kacmarek RM, Dimas B, Reynolds J, Shapiro BA (1982) Technical aspects of positive end-expiratory pressure (PEEP). III. PEEP with spontaneous ventilation. Respir Care 27:1505–1517
Branson RD (1993) The nuts and bolts of increasing arterial oxygenation: devices and techniques. Respir Care 38:672–686
Younes M, Puddy A, Roberts D, Light RB, Quesada A, Taylor K, Oppenheimer L, Cramp H (1992) Proportional assist ventilation. Am Rev Respir Dis 145:121–129
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Konyukov, Y.A., Kuwayama, N., Fukuoka, T. et al. Effects of different triggering systems and external PEEP on trigger capability of the ventilator. Intensive Care Med 22, 363–368 (1996). https://doi.org/10.1007/BF01700461
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01700461