Abstract
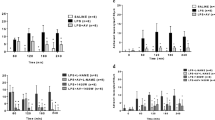
Objective: Endotoxin rapidly inhibits the activity of the constitutive endothelial nitric oxide synthase (ecNOS); this precedes the production of NO from inducible NOS (iNOS). This leaves a period in early endotoxaemia with a supposed scarcity of NO. The present study was conducted to examine the effects of external supplementation of NO on liver microcirculation and function. Material: 13 male Sprague Dawley rats. Interventions: The rats underwent laparotomy, and the left liver lobe was exteriorised. All animals were given a bolus dose of endotoxin (LPS) 5 mg/kg intraportally. One group (n = 6) had a continuous infusion of sodium nitroprusside (SNP) 1.4 μg/kg per min started concurrently, the other group (n = 7) was treated with normal saline. The study was terminated after 3 h LPS. Measurements and results: Intravital microscopy was performed at baseline, at 2 h and 3 h LPS. Hepatic function was assessed by arterial ketone body ratio, acid base values, and bile flow. At baseline 1 % of the sinusoids were without perfusion. After 2 h LPS this figure had risen to 9.8 ± 1.5 % in the SNP group versus 16.9 ± 1.4 % in the controls (p < 0.05 vs controls). The corresponding values after 3 h LPS were 13.5 ± 1.5 versus 19.3 ± 1.5 % (p < 0.05 vs controls). The leukocyte count in sinusoids and venules had a similar development. Functional parameters were all slightly better preserved in the SNP group, but with no individual significance versus controls. Conclusions: Infusion of the NO donor SNP in early endotoxaemia attenuates the detrimental effects of LPS on liver microcirculation, most probably by alleviating a relative deficit of NO at the microcirculatory level.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Received: 19 February 1998 Accepted: 2 September 1998
Rights and permissions
About this article
Cite this article
Gundersen, Y., Corso, C., Leiderer, R. et al. The nitric oxide donor sodium nitroprusside protects against hepatic microcirculatory dysfunction in early endotoxaemia. Intensive Care Med 24, 1257–1263 (1998). https://doi.org/10.1007/s001340050759
Issue Date:
DOI: https://doi.org/10.1007/s001340050759