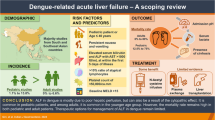
Abstract
The clinico-pathological entity of flucloxacillin-associated cholestatic hepatitis is described and the recognition and documentation of cholestasis associated with flucloxacillin and with related isoxazolyl-penicillins (cloxacillin, dicloxacillin) is examined on an international basis, with particular reference to Australia. Data were obtained from the literature, from the Australian adverse drug reaction monitoring agency and from the Collaborative Centre for International Drug Monitoring (World Health Organisation) in Sweden. Approximately 600 cases of flucloxacillin-associated cholestatic hepatitis were collected, as well as 164 cases associated with other isoxazolyl penicillins.
Jaundice and pruritus may first appear several weeks after administration of the drug has ceased and typically are severe and protracted. Liver tests may be abnormal for months after symptomatic recovery. Death is uncommon. Liver pathology shows centrizonal bile stasis with portal tract inflammation and variable loss of bile ducts. Approximately 1 in 15,000 users of flucloxacillin will develop the reaction. Increasing age (>55 years) and prolonged intake (>14 days) are particular risk factors. Cholestasis associated with cloxacillin/dicloxacillin appears to be similar in nature but is less well defined. Recognition and reporting of the reaction have been uncommon in the United Kingdom inter alia and high in Sweden and Australia, although estimates of risk have been similar. In Australia, the remarkably high rate of reports appears to be the result of sustained publicity for the reaction. There is only a trickle of reports of cholestatic hepatitis in association with the use of cloxacillin and dicloxacillin from the USA and Canada. The high level of awareness of the reaction and consequential regulatory action so far have not resulted in a diminution of its occurrence in Australia.
Similar content being viewed by others
References
Hoigne R, Keller H, Sonntag (1988) Penicillins, cephaslosporins and tetracyclines. In: Dukes MNG, (ed). Meyler's side effects of drugs. Elsevier, Amsterdam, pp 501–542
Tem pas A, Quinn EL (1965) Cholestatic hepatitis following the administration of sodium oxacillin. JAMA 191:138–139
Berger M, Potter DE (1977) Pitfalls in diagnosis of viral hepatitis on a haemodialysis unit. Lancet 2:95–96
Enat R, Pollak S, Ben-Areh Y, Livni E, Baszilai D (1980) Cholestatic jaundice caused by cloxacillin: macrophage inhibition factor test in preventing rechallenge with hepatic toxic drugs. Br Med J 1:982–983
Onorato IM, Axelrod JL (1978) Hepatitis from intravenous high dose oxacillin therapy: findings in an adult inpatient population. Ann Intern Med 89:497–499
Pollak AA, Berger SA, Simberkoff MS, Rahal Jr JJ (1978) Hepatitis associated with high dose oxacillin therapy. Arch Intern Med 138:195–197
Bengtsson F, Floren CH, Hagerstrand I, Soderstrom C, Aberg T (1985) Flucloxacillin induced cholestatic liver damage. Scand J Infect Dis 17:125–128
Victorino RMM, Maria BA, Correia AP, de Moura C (1987) Flucloxacillin induced cholestatic hepatitis with evidence of lymphocyte sensitisation. Arch intern Med 147:987–989
Deboever G (1987) Cholestatic jaundice due to derivatives of oxacillin (letter) Am J Gastroenterol 82:483
Turner IB, Eckstin RP, Riley JW, Lunzer MR (1989) Prolonged hepatic cholestasis after flucloxacillin therapy. Med J Austr 151:701–705
Miros M, Kerlin P, Walker N, Harris O (1990) Flucloxacillin induced delayed cholestatic hepatitis. Aust NZ J Med 20:251–253
Swedish Adverse Drug Reactions Advisory Committee Bulletin (1989) Flucloxacillin and liver damage. No 54
Australian Adverse Durg Reactions Bulletin (1990) Flucloxcillin hepatitis. February
Australian Adverse Drug Reactions Bulletin (1990) Flucloxacillin hepatitis. November
Committee on Safety of Medicines (1992) Flucloxacillin induced cholestatic jaundice. Current Problems No. 35, Nov.2
Australian Adverse Drug Reactions Bulletin (1992) Update on flucloxacillin hepatitis. February
Adverse Drug Reactions Advisory Committee of the Australian Drug Evaluation Committee (1992) Drug induced cholestatic hepatitis common antibiotics. Med J Austr 157:531
Olsson R, Wiholm BE, Sand C, Zettergren L, Hultcrantz R, Myrhed M (1992) Liver damage from flucloxacillin, cloxacillin and dicloxacillin. J Hepatol 15:154–161
Fairley CK, Boyd I, Purcell P, McNeil J (1992) Flucloxacillin jaundice (Letter). Lancet 339:679
Australian Adverse Drug Reactions Bulletin (1994) Fatal hepatic reactions to flucloxacillin. August
Lobatto S, Dijkmans BAC, Mattie M, Van Hooff JP (1982) Flucloxacillin associated liver damage. Neth J Med 25:47–48
Tauris P, Jorgensen NF, Petersen CM, Albertsen K (1985) Prolonged severe cholestasis induced by oxacillin derivatives. Acta Med Scand 217:567–569
Eckstein RP, Dowsett JF, Lunzer MR (1993) Flucloxacillin induced liver disease: histopathological findings at biopsy and autopsy. Pathology 25:223–228
Davies MH, Harrison RF, Elias E, Hübscher SG (1994) Antibiotic-associated acute vanishing bileduct syndrome: a pattern associated with severe, prolonged intrahepatic cholestasis. J Hepatol 20:112–116
Fairley CK, MacNeill JJ, Desmond P, Smallwood R, Young H, Forbes A, et al (1993) Risk factors for development for flucloxacillin associated jaundice. Br Med J 306:233–235
Derby LE, Jick H, Henry DA, Dean AD (1993) Cholestatic hepatitis associated with flucloxacillin. Med J Austr 158: 596–600
Australian Drug Evaluation Committee (1987) Report of suspected adverse drug reactions No. 6. Aust Govt Publishing Service, Canberra
Derby LE, Jick H, Henry DA, Dean AD (1993) Erythromycin-associated cholestatic hepatitis. Med J Austr 158:600–602
Keller H, Follath F (1988) Miscellaneous antibiotics. In: Dukes MNG (ed) Meyler's side effects of drugs. Elsevier Amsterdam, pp 543–566
Jick H, Desley LE, Dean AD, Henry DA (1994) Flucloxacillin and cholestatic hepatitis. Med J Austr 160:525
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Crawford, D.H.G., Roeser, H.P., Devereaux, B.M. et al. Flucloxacillin associated cholestatic hepatitis. Eur J Clin Pharmacol 49, 81–85 (1995). https://doi.org/10.1007/BF00192363
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00192363