Abstract
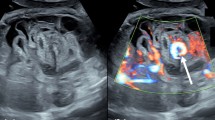
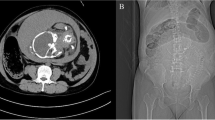
This article describes a prenatal ultrasonographic finding of an infarcted intestinal volvulus. Ultrasonography showed polyhydramnios, multiple dilated intestinal loops, increased transverse abdominal area, and ascites. After cesarean section due to premature rupture of membranes and fetal distress, derotation of the infarcted volvulus caused postoperative thrombocytopenia, hyperkalemia, and acidosis and a subsequent resection was required. A high output of intestinal juice from the jejunostomy caused severe hypovolemia and electrolyte imbalance with resultant death. Increased transverse abdominal area caused by marked intestinal dilatation, ascites, fetal distress, and hydrops fetalis may suggest an infarcted intestinal volvulus.
Similar content being viewed by others
References
Chiba Y (1985) Ultrasound diagnosis of fetal growth. In: Chiba Y (ed) Ultrasound in obstetrics and gynecology. Kinpodo, Kyoto, pp 67–79
Fleischer AC, Goldstein RB, Bruner JP, Worrell JA (1994) Doppler sonography in obstetrics and gynecology. In: Callen PW (ed) Ultrasonography in obstetrics and gynecology. WB Saunders Co, Philadelphia, pp 503–523
Ho Mmed NK, Cheah SL, Ong CL (1990) In utero intestinal volvulus presenting as neonatal emergency. J Singap Paediatr Surg 32: 149–151
Seward JF, Zusman J (1978) Hydrops fetalis associated with small-bowel volvulus. Lancet 1: 52–53
Stringel G, Gillieson M, Muram D, Mercer S (1983) Perinatal management of major gastrointestinal anomalies by maternal ultrasound. Clin Pediatr 22: 564–566
Suzumori K, Adachi R, Yagami Y, Hajime Togari (1990) A fetal case with midgut volvulus. Asia-Oceania J Obstet Gynecol 16: 13–16
Witter FR, Molteni RA (1986) Intrauterine intestinal volvulus with hemoperitoneum presenting as fetal distress at 34 weeks' gestation. Am J Obstet Gynecol 155: 1080–1081
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hasegawa, T., Yoshioka, Y., Sasaki, T. et al. Infarcted intestinal volvulus detected by prenatal ultrasonography. Pediatr Surg Int 11, 498–499 (1996). https://doi.org/10.1007/BF00180094
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF00180094