Abstract
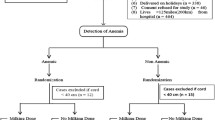
Blood volume and its components were estimated using 125iodinated human serum albumin in 194 newborn infants with 26 to 41 week gestations. Umbilical cords were ligated 15 seconds after vaginal delivery (n=141) and within 5 seconds after delivery by Caesarean section (n=53). The infants were divided into four groups according to the mode of delivery and presence of prenatal complications: group I: vaginal deliveries (n=96) and group II: Caesarean section (n=25) without preceding complications; group III: infants with intra-uterine asphyxia (n=56); group IV: infants with tight umbilical cord loops around neck (n=17). Subgroups were established with respect to gestational age and to one-minute Apgar scores. Significantly different blood volume (BV) and red cell mass (RCM) values between the subgroups were only found in group I with respect to different Apgar scores: Ia Apgar>5: BV 77.9±6.2; RCM 37.5±5.1 ml/kg; Ib Apgar<6: BV 70.0±4.4; RCM 29.6±2.9 ml/kg (P<0.005). Intra-partum asphyxia did not affect BV (71.3±4.8 ml/kg) and RCM (31.2±3.6 ml/kg) in group II. BV and RCM were significantly (P<0.005) lower than in group Ia. In group III, BV (90.4±7.0 ml/kg) and RCM (46.9±6.3 ml/kg) were significantly (P<0.005) higher than in group I, irrespective of the mode of delivery and Apgar scores. The infants of group IV had the lowest volumes (BV 67.5±5.7; RCM 27.4±2.7 ml/kg). Values obtained in premature and full-term infants were similar in the respective groups. These results indicate that infants with intra-partum asphyxia and with tight nuchal cords do not participate in placental transfusion or even lose some blood into the placenta. However, infants with intrauterine asphyxia (excepting those with tight nuchal cords) receive marked placental transfusion in utero.
Similar content being viewed by others
References
Bissonnette, J. M.: Control of vascular volume in sheep umbilical circulation. J. Appl. Physiol. 38, 1057–1061 (1975)
Brown, E. G., Krouskop, R. W., McDonnell, F. E., Sweet, A. Y.: Blood volume and blood pressure in infants with respiratory distress. J. Pediatr. 87, 1133–1138 (1975)
Cashore, W. J., Usher, R. H.: Hypovolemia resulting from a tight nuchal cord at birth. Pediatr. Res. 7, 399 (1973)
Celander, O.: Studies of the peripheral circulation. In: The heart and circulation in the newborn and infant (ed. D. E. Cassels), pp. 98–110. New York: Grune and Stratton 1966
Celander, O., Mårild, K.: Reactive hyperemia in the foot and calf of the newborn infant. Acta Paediatr. Scand. 51, 544–552 (1962)
Chou, P. J., Ackerman, B. D.: Permatal acidosis and placental transfusion. Acta Paediatr. Scand. 62, 417–422 (1973)
Cohn, H. E., Sacks, E. J., Heymann, M. A., Rudolph, A. M.: Cardiovascular responses to hypoxemia and acidemia in fetal lambs. Am. J. Obstet. Gynecol. 120, 817–824 (1974)
Dawes, G. S.: The umbilical circulation. Am. J. Obstet. Gynecol. 84, 1634–1648 (1962)
Dawes, G. S., Lewis, B. V., Milligan, J. E., Roach, M. R., Talner, N. S.: Vasomotor responses in the hind limbs of foetal and new-born lambs to asphyxia and aortic chemoreceptor stimulation. J. Physiol. (Lond.) 195, 55–81 (1968)
Faxelius, G., Raye, J., Gutberlet, R., Swanstrom, S., Tsiantos, A., Dolanski, E., Dehan, M., Dyer, N., Lindstrom, D., Brill, A. B., Stahlman, M.: Red cell volume measurements and acute blood loss in high-risk newborn infants. J. Pediatr. 90, 273–281 (1977)
Flod, N. E., Ackerman, B. D.: Perinatal asphyxia and residual placental blood volume. Acta Paediatr. Scand. 60, 433–436 (1971)
Hon, E. H., Quilligan, E. J.: The classification of fetal heart rate. II. A revised working classification. Conn. Med. 31, 779–784 (1967)
Kitterman, J. A., Schlueter, M. A.: Effects of intra-uterine asphyxia on neonatal blood volume. Pediatr. Res. 8, 173 (1974)
Klebe, J. G., Ingomar, C. J., Nørgaard-Pedersen, B.: Blood volumes in premature infants of diabetic and non-diabetic mothers, correlated with the time of clamping of the umbilical cord. Acta Paediatr. Scand. 61, 549–554 (1972)
Kleinberg, F., Phibbs, R., Dong, L.: Lack of placenta to infant transfusion with delayed cord clamping after Caesarean section delivery. Pediatr. Res. 7, 403 (1973)
Linderkamp, O., Holthausen, H., Seifert, J., Butenandt, I., Riegel, K. P.: Accuracy of blood volume estimations in critically ill children using 125I-labelled albumin and 51Cr-labelled red cells. Europ. J. Pediatr. 125, 143–151 (1977)
Linderkamp, O., Mader, T., Butenandt, O., Riegel, K. P.: Plasma volume estimation in severely ill infants and children using a simplified Evans blue method. Europ. J. Pediatr. 125, 135–141 (1977)
Linderkamp, O., Fendel, H., Versmold, H. T., Riegel, K. P., Betke, K.: Association of neonatal respiratory distress with birth asphyxia and red cell mass deficiency in premature infants. Europ. J. Pediatr. (submitted)
Mann, L. I.: Effects of hypoxia on umbilical circulation and fetal metabolism. Am. J. Physiol. 218, 1453–1458 (1970)
McCue, C. M., Garner, F. B., Hurt, W. G., Schelin, E. C., Sharpe, A. R.: Placental transfusion. J. Pediatr. 72, 15–21 (1968)
Messow-Zahn, K., Sarafoff, M., Riegel, K. P.: Stress at birth: Plasma noradrenaline concentrations of women in labour and in cord blood. Klin. Wochenschr. (in press)
Milligan, J. E., Roach, M. R., Talner, N. S.: Vasomotor responses in the hindlimb of newborn calves. Circ. Res. 21, 237–244 (1967)
Moinian, M., Meyer, W. W., Lind, J.: Diameters of umbilical cord vessels and the weight of the cord in relation to clamping time. Am. J. Obstet. Gynecol. 105, 604–611 (1969)
Neligan, G. A., Oxon, D. M., Smith, C. A.: The blood pressure of newborn infants in asphyxial states and in hyaline membrane disease. Pediatrics 26, 735–744 (1960)
Oh, W., Blankenship, W., Lind, J.: Further study of neonatal blood volume in relation to placental transfusion. Ann. Paediatr. 207, 147–159 (1966)
Omori, K., Phelps, D. L., Emmanouilides, G. C., Oh, W.: Placenta to fetus transfusion in utero during acute hypoxemia in fetal lamb. Pediatr. Res. 7, 168 (1973)
Philip, A. G. S., Yee, A. B., Rosy, M., Surti, N., Tsamtsouris, A., Ingall, D.: Placental transfusion as an intrauterine phenomenon in deliveries complicated by foetal distress. Brit. Med. J. II, 11–13 (1969)
Saigal, S., O'Neill, A., Surainder, Y., Chua, L.-B., Usher, R.: Placental transfusion and hyperbilirubinemia in the premature. Pediatrics 49, 406–419 (1972)
Scheffé, H.: A method for judging all contrasts in the analysis of variance. Biometrika 40, 87–104 (1953)
Sisson, T. R. C., Knutson, S., Kendall, N.: The blood volume of infants. IV. Infants born by Caesarean section. Am. J. Obstet. Gynecol. 117, 351–357 (1973)
Usher, R., Lind, J.: Blood volume of the newborn premature infant. Acta Paediatr. Scand. 54, 419–431 (1965)
Usher, R. H., Saigal, S., O'Neill, A., Surainder, Y., Chua, L.-B.: Estimation of red blood cell volume in premature infants with and without respiratory distress syndrome. Biol. Neonate 26, 241–248 (1975)
Usher, R., Shephard, M., Lind, J.: The blood volume of the newborn infant and placental transfusion. Acta Paediatr. Scand. 52, 497–512 (1963)
Yao, A. C., Hirvensalo, M., Lind, J.: Placental transfusion-rate and uterine contraction. Lancet 1, 380–383 (1968)
Yao, A. C., Lind, J.: Effect of gravity on placental transfusion. Lancet 2, 505–508 (1969)
Yao, A. C., Lind, J.: Blood volume in the asphyxiated term neonate. Biol. Neonate 21, 199–209 (1972)
Yao, A. C., Lind, J., Tiisala, R., Michelsson, K.: Placental transfusion in the premature infant with observation on clinical course and outcome. Acta Paediatr. Scand. 58, 561–566 (1969)
Yao, A. C., Moinian, M., Lind, J.: Distribution of blood between infant and placenta after birth. Lancet 2, 871–873 (1969)
Yao, A. C., Wist, A., Lind, J.: The blood volume of the newborn infant delivered by Caesarean section. Acta Paediatr. Scand. 56, 585–592 (1967)
Author information
Authors and Affiliations
Additional information
Supported by Deutsche Forschungsgemeinschaft, SFB 147
Rights and permissions
About this article
Cite this article
Linderkamp, O., Versmold, H.T., Messow-Zahn, K. et al. The effect of intra-partum and intra-uterine asphyxia on placental transfusion in premature and full-term infants. Eur J Pediatr 127, 91–99 (1978). https://doi.org/10.1007/BF00445764
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF00445764