Summary
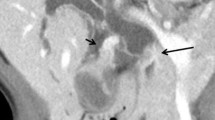
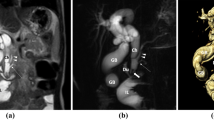
We report, in an adult, an asymptomatic association between cystic dilatation of the bile duct (type IV A in Todani's classification) and anomalous pancreatico-biliary ductal union (APBD) with stones in a long common channel. In APBD, the connection between the common bile duct and the main pancreatic duct is located outside the duodenal wall and is therefore not under the influence of the sphincter of Boyden. An abnormally long common channel is in excess of 15 mm. Two types of convergence anomalies are defined according to whether the bile duct opens into the main pancreatic duct (BP) or the main pancreatic duct into the bile duct (PB). In APBD, there is probably a reverse pressure gradient between the bile and pancreatic ducts, with regurgitation of pancreatic juice into the bile duct, repeated attacks of cholangitis, stenosis and cystic dilatation. A long common channel is associated with a higher incidence of carcinoma of the gall bladder or the bile duct.
Résumé
Nous rapportons, chez l'adulte, une association asymptomatique d'un kyste cholédocien (type IV A de la classification de Todani) et d'une anomalie de la convergence bilio-pancréatique (APBD), avec présence de calculs dans un canal commun long. En présence d'APBD, la réunion entre la voie biliaire principale et le conduit pancréatique se fait en dehors de la paroi duodénale et échappe au contrôle du sphincter hépato-pancréatique. Un canal commun long est considéré comme pathologique s'il est > 15 mm. S'il apparît que le canal pancréatique vient se jeter dans la voie biliaire, cette anomalie correspond au type P-B. S'il s'agit du canal cholédocien qui vient se jeter dans la voie pancréatique, l'anomalie est de type B-P. Dans ces anomalies de la convergence bilio-pancréatique, il est probable qu'il existe une inversion du gradient de pression bilio-pancréatique avec reflux de liquide pancréatique dans les voies biliaires engendrant cholangite, sténose et dilatation kystique. Un canal commun bilio-pancréatique long est associé, avec une grande fréquence, un cancer de la vésicule ou des voies biliaires.
Similar content being viewed by others
References
Arnolds (1906) Eine manneskopfgrosse Retentionszyste des Choledochus. Dtsch Med Wochenschr 32: 1804
Babbitt DP, Starshack RJ, Clemett AR (1973) Choledochal cyst: a concept of etiology. Am J Roentgenol 119: 57–62
Bolognini B, Marchand JP, Pariente EA., Viala JF, Kapfer J, Grossetti D, Trinh DH (1993) Dilatation kystique asymptomatique du cholédoque chez un adulte. Gastroenterol Clin Biol 17: 292–2944
Caroli J, Soupault R, Kossakowski J, Plocker L, Paradowska M (1958) la dilatation polykystique congénitale des voies biliaires intrahépatiques. Essai de classification. Sem Hop Paris 34: 488–495
Dunham F, Engelhom I, Toussaint J, Deltenre M, Lambilliotte JP, Cremer M (1981) Investigation des dilatations kystiques idiopathiques du cholédoque par cholangio-pancréatographies. Acta Gastro Enterol Belg 44: 274–283
Flanigan DP (1975) Biliary cysts. Ann Surg 182: 635–643
Jona JZ, Babbitt DP, Starshak RJ, La Porta AJ, Glicklich M, Cohen RD (1979) Anatomic observations and etiologic and surgical considerations in choledochal cyst. J Paediatr Surg 14: 315–320
Kato O, Hattori K, Suzuki T, Tachino F, Yuasa T (1983) Clinical significance of anomalous pancreaticobiliary union. Gastrointest Endosc 29: 94–98
Kimura K (1976) Studies in 28 cases of congenital cystic dilatation of the common bile duct in adults. Roentgenological features and a union between the choledochus and the main pancreatic duct. Jpn J Gastroenterol 73: 61–74
Kimura K, Ohto M, Saisho H (1985) Association of gallbladder carcinoma and anomalous pancreaticobiliary duct union. Gastroenterology 89: 1258–1265
Komi N (1975) Anomalous arrangement of pancreaticobiliary duct. Shuzustsu 29: 73–83
Komi N, Kashiwagi Y, Ikeda N (1977) The etiology of congenital dilatation of the biliary duct. Jpn J Paediatr Surg 9: 1101–1109
Kozloff L, Joseph WL (1973) Cystic dilatation of the commun bile duct in adults. Med Ann 42: 595
Lee SP, La mont JT, Carey MC (1981) Role of gall bladder mucus hypersecretion in the evolution of cholesterol gall stones. J Clin Invest 67: 1712–1723
Lucas St, Verhaeghe P, Stoppa R (1986) Le syndrome du canal commun associé à une dilatation kystique de la voie biliaire principale. A propos d'un cas compliqué de lithiase du canal commun. J Chir 123: 490–496
Misra SP, Dwivedi M (1990) Pancreaticobiliary ductal union. Gut 31: 1144–1149
Misra SP, Gulati P, Thorat VK, Vij JC, Anand BS (1989) Pancreatico-biliary ductal union in biliary diseases. An endoscopic retrograde cholangiopancreaticographic study. Gastroenterology 96: 907–912
Nagorney DM, Mc Ilrath DC, Adson MA (1984) Choledochal cysts in adults: clinical management. Surgery 96: 656–663
Ono J, Sakoda K, Akita H (1982) Surgical aspect of cystic dilatation of the bile duct. Ann Surg 195: 203–208
Sénèque J, Tailhefer A (1929) Les dilatations congénitales du cholédoque: anciens kystes idiopathiques du cholédoque. J Chir 33: 154–178
Todani T, Watanabe J, Narusue M, Tabuchi K, Okajima K (1977) Congenital bile duct cysts. Classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg 134: 263–269
Womack N, Zeppa R, Irvin G (1963) The anatomy of gallstones. Ann Surg 157: 670–686
Wong KC, Lister J (1981) Human foetal development of hepatopancreatic duct junction — a possible explanation of congenital dilatation of the biliary tract. J Paediatr Surg 16: 139–145
Yamaguchi M (1980) Congenital choledochal cyst. Analysis of 1433 patients in the Japanese literature. Am J Surg 140: 653–657
Yotsuyanagi S (1935) Contribution to etiology and pathology of idiopathic cystic dilatation of the common bile duct, with report of three cases. Gann 30: 601–656
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Richer, J.P., Faure, J.P., Morichau-Beauchant, M. et al. Anomalous pancreatico-biliary ductal union with cystic dilatation of the bile duct. Surg Radiol Anat 20, 139–142 (1998). https://doi.org/10.1007/BF01628919
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01628919